Doctors and nurses are often the main people we think of when it comes to those treating COVID-19 patients. I work with some incredible doctors and nurses, alongside a number of other healthcare professionals on the wards. There are Health Care Assistants (HCA’s), physiotherapists, occupational therapists, speech & language therapists, psychologists, palliative care teams, dietitians, discharge co-ordinators, cleaners, catering staff, and so many more people caring for patients and ensuring the smooth running of the hospital.
When I initially wrote this post, I wanted to share more about what dietitians were doing (following on from my instagram post!). But as I was writing and posting on IG, I was getting messages from other Allied Health Professionals saying thank you for talking about them. And so this blog morphed into a much longer post, sharing more about AHP’s on the frontline
I feel like I’ve learned so much about my colleagues. There’s such a feeling of collaboration in my hospital right now, more than eve. And I’m working alongside teams I haven’t come into contact with before. Everyone wearing scrubs has actually been a great way of getting rid of hierarchy!
Allied Health Professionals in the Response to Coronavirus
I spoke with the teams that I work alongside at the hospital as well as asking on Instagram for those working for the NHS what their job roles are, how they’ve changed and what they are doing on the front lines currently. This is by no means exhaustive. So if you’re working in health care right now, I would love to hear about your job in the comments!
Physiotherapists
Thea is working as an NHS rotational physiotherapist (this means that they swap speciality usually every 6/12 months), and is currently working on respiratory. Previously she was working on ICU and the Ear Nose and Throat surgical ward. However, now she’s just based on Intensive Care. Their roles have changed not only to help patients, but to support the very overstretched nursing staff on the units.
Within the ICU, one of the main role of physios is to prone patients (lie them on their fronts) to aid with ventilation. Proning an intubated, sedated and paralysed patient requires up to five members of staff to turn them safely, including an airway trained doctor to hold the intubation tube during the process. Physiotherapists are well trained to help with the safe proning of patients as they have a lot of experience with manual handling, and positioning/alignments of patients to ensure prevention of loss of range and protection of pressure areas (eg heels, buttocks).
When not helping to prone patients, we are helping to reposition patients, treating their chests (eg clearing secretions) and providing rehab for patients as part of our normal therapy provision. We’re also working hard to support the nursing staff. Eg helping with donning and doffing of PPE (personal protective equipment), being ‘runners’ outside sealed bays to fetch things they need, etc.
As the virus progresses, and patients are weaned off ventilation, physios will play a key role in rehabilitation as they overcome ICU-acquired weakness (patients tend to lose a lot of weight and muscle mass during ICU stays, despite feeding them!). Patients are being treated post-COVID are helped to ‘manage their chest and clear secretions when they’re too weak to do it themselves’. Many patients are very weak, vulnerable and exhausted during recovery. And so they are given time to recover and support with this. To give an example, some patients are finding it extremely tiring just sitting up in a chair for longer than 15 minutes.
Many physiotherapists have changed from a 5 day week, to a 7 day working week. Covering days and nights to cope with demand.
Laura is a community physiotherapist, as well as working ‘on call’ at the hospital and covering weekends. She explained that many of her non-urgent patients are being reviewed via telephone consultations (rather challenging!). And only urgents are seen face-to-face with PPE. A lot of their community patients are in the extremely vulnerable category with multiple co-morbidities and trying to protect them is key. However they still need crucial items such as walking aids to prevent falls and reduce hospital admissions.
Occupational Therapists
I’m friends with a couple of the OT’s on the wards I work on. And have had the opportunity to get to know a lot more about their role in safe patient discharge. Alongside the OT’s that I work with, I also spoke to a couple of Occupational Therapists on IG including Cassie, an OT working on a hyperacute and acute stroke unit.
An OT’s role is to assess, rehab and discharge patients home safely. This hasn’t changed during COVID however the timeframe with which discharges are happening has! They assess patients deficits post incident/event and how this impacts a persons ability to complete everyday tasks ranging from feeding themselves, washing and dressing, to driving and working. They then will work with a patient in rehabilitation to aid them back to independence.
Wearing PPE all days makes sessions with patients harder for both staff and patients. (Some confused patients must be quite terrified.)
Many OT’s have been upskilled to assist with tasks such as proning. So they can be redeployed if/when needed. I spoke to Kerry, another Specialist OT in Acute stroke and Neurosciences. Her role has changed greatly within the hospital since COVID. Including providing weekend cover, so that patients can be rehabilitated post critical care and on general wards. The rehab OT’s are currently providing has changed somewhat. They are working with all ages but the rehabilitation is very slowly, focusing on fatigue and gently grading rehabilitation intensity everyday. Staff from paediatrics OT have been redeployed to support adult OT’s and retired occupational therapists have voluntarily returned to the frontline.
Kerry told me that Although she is a specialist in the neuro field, she’s seeing patients from all areas such as medicine for the elderly (frailty), respiratory, cardiology. “I feel I have learnt a lot of new skills and our department as a whole have all worked together to up skill everyone. So in this pandemic there are many positives and a department that has pulled together to help and support each other. Whilst on the COVID wards I have helped nursing staff with routine washes, toileting patients and even learnt a new skill of completing OBS and filling out NEWS charts. I have helped patients set up mobile phones to enable them to call or FaceTime their families. The key has been I am still doing my job as an Occupational Therapist but doing my best to support the nursing staff as best I can.”
Cassie told me ‘ it’s so important for the public to know that the NHS is still open and that although the covid crisis is going on, we are still there to help those that have a life changing diagnosis’.
Speech and Language Therapists
My friend Ellie is a SLT, and I’ve learned a lot about what they actually do over the last few years. Speech and Language teams work on the specialist assessment and treatment of communications problems from either a condition (eg stroke) or from treatment (eg intubation damage to vocal cords or tracheostomy). They also work on the management of swallowing problems. Including too much or too little saliva, difficulty drinking fluids, eating textured foods and taking medications. This is called dysphagia and here they work alongside dietitians to ensure patients have adequate, safe nutrition.
SLT’s are trained to support clinical decisions for weaning patients off their ventilators or tracheostomy tubes. Something that is very prevalent currently during COVID. Most patients admitted to ICU currently are requiring ventilation, some for a long time. The longer a patient is ventilated, the higher the risk of damage to larynx which can lead to voice problems and dysphagia.
As mentioned above, patients lose a lot of muscle mass on intensive care. This not only affects arms and legs, but the muscles that are used for speech and swallowing. At its most severe, patients aren’t able to swallow their own saliva. Similarly, when patients are short of breath (a characteristic of COVID), breathing and swallowing patterns are disrupted, which can lead to dysphagia.
Due to all the PPE that staff are having to wear to treat patients, communication is difficult. (Especially for patients with hearing impairments, cognitive impairments and those who don’t speak English.) Ellie and her team are providing resources to nurses and doctors to help facilitate communication between themselves and their patients.
Health Care Assistants
HCA’s typically work alongside nurses on the wards, assisting with patients washing and dressing patients, ensuring their comfort and safety, helping during mealtimes, as well as helping patients with bathroom needs. They chat with patients, keep them calm which is especially crucial right now with patients on breathing machines (I saw two HCA’s holding the hands of a gentleman as he struggled to breathe on the ward last week).
I also spoke with an HCA at a GP surgery who explained that she’s involved with monitoring and sourcing PPE as well as writing guidance protocols for appropriate usage of PPE. She’s also providing additional cleaning and decontamination, assisting with doctors examining patients to prevent cross-contamination of equipment.
Radiographers
A radiographer on instagram messaged me to explain how they are involved with the treatment of COVID patients. And I have to admit, I don’t come into contact with radiographers at work. So it’s a profession I don’t know much about at all.
He explained that although their roles have remained widely unchanged, they are a lot busier. All covid patients are imaged when they arrive through A and E. And then continuously throughout their stays having daily xrays/ct scans. Like a lot of those working in specialities, they have to spend their whole day in PPE as we image itubated patients. They are also now spending hours in ITU/wards carrying out daily xrays to check on chest condition.
Whilst they have this added workload, they are still proving imaging to all other patients. E.g. stroke patients, trauma patients, oncology patients. Our Radiographers continue to cover x-rays, CT scans, MRI scans, IR procedures such as thrombectomies, RIGS,nephrostomies etc. Most patients who enter the hospital will have contact with Radiographer!
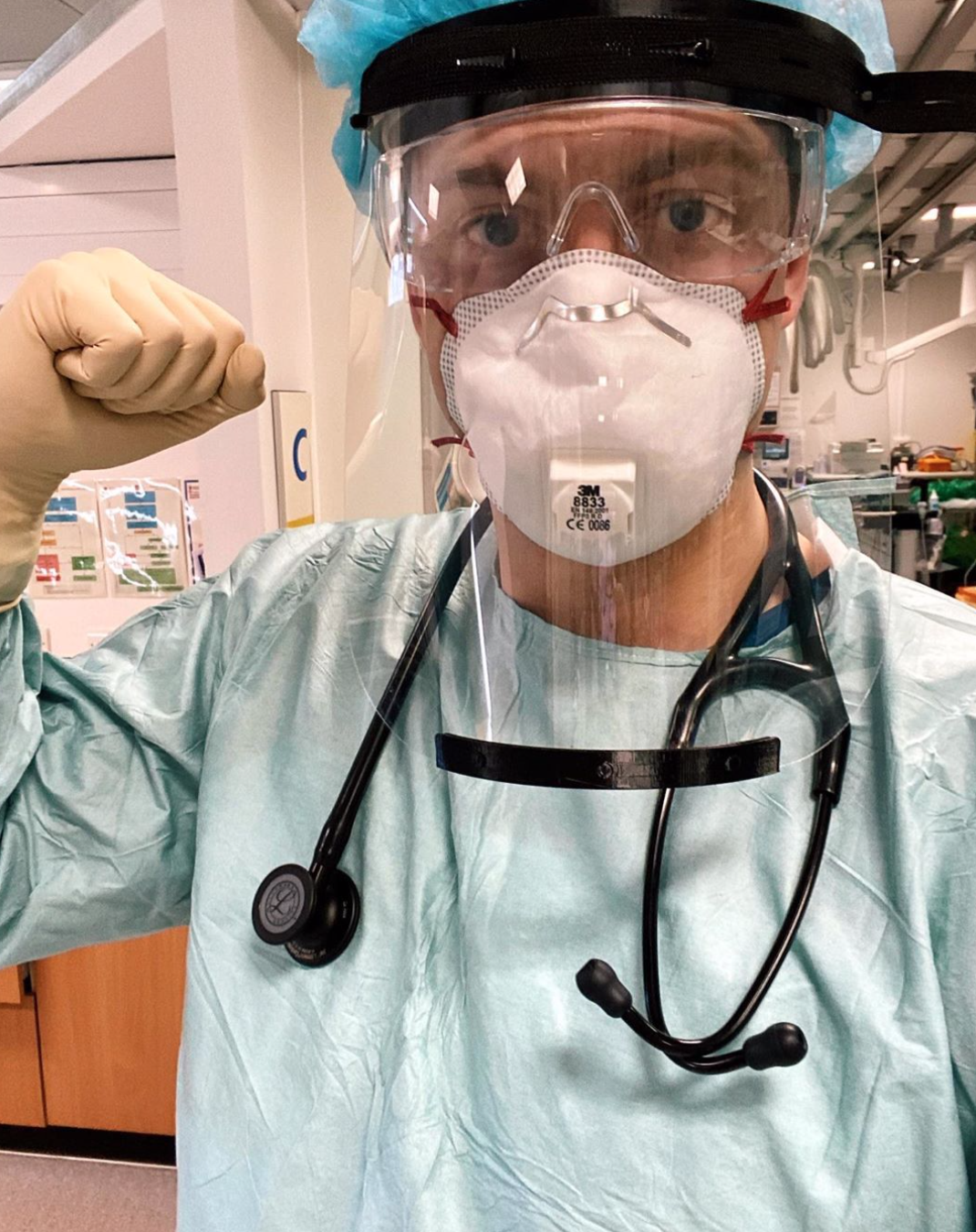
A note on PPE… there are different levels of PPE (sharing a pic of Dr Alex because I’m not allowed to share photos of myself in PPE). I have to wear full PPE on three of the wards that I go on. And I am amazed at how those working on those wards full time are managing. It is so hot and almost suffocating within all the layers. And very difficult to communicate with patients through the mask and shield.
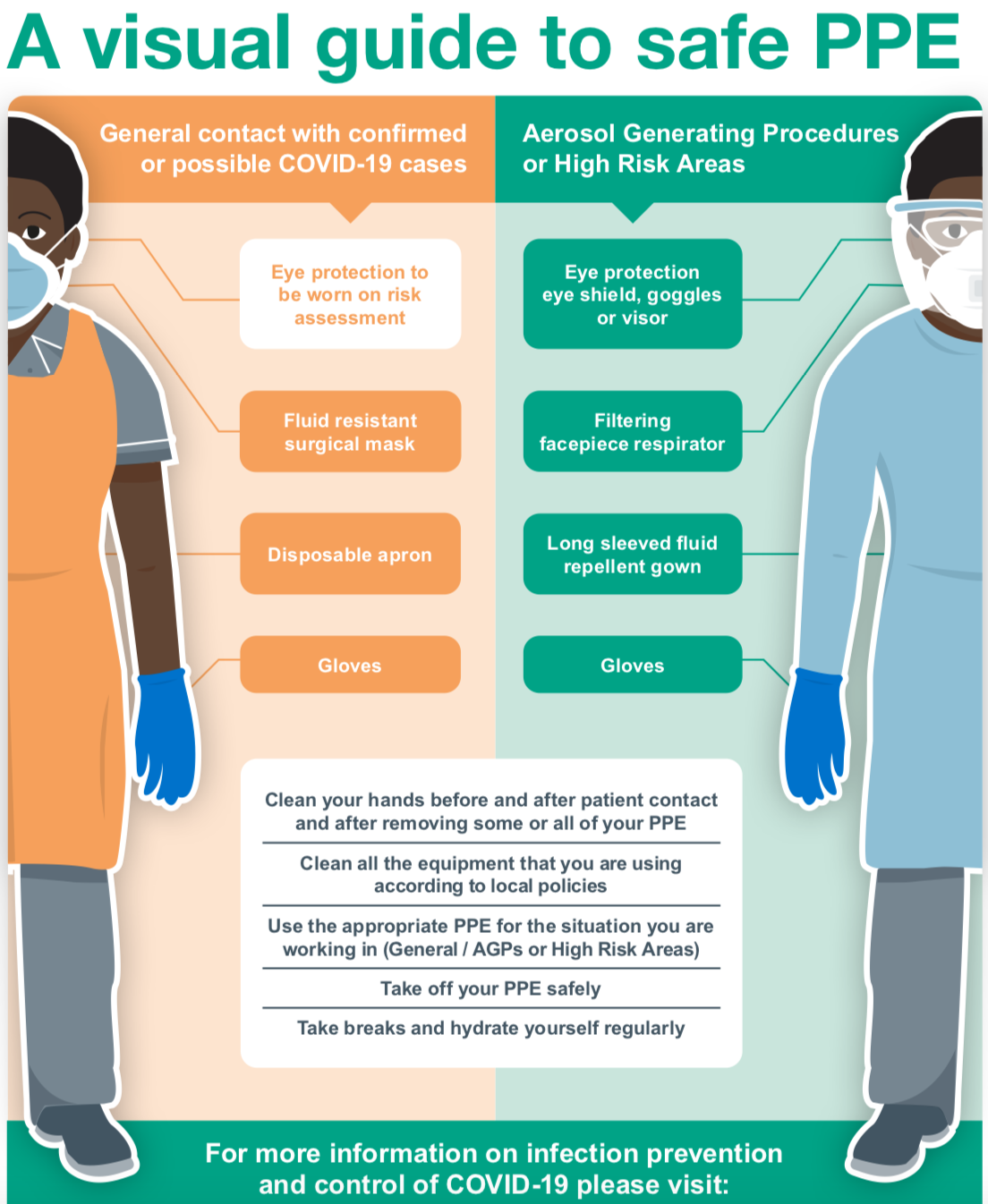
FULL PPE -> this is worn during aerosol generating procedures, when patients are intubated and ventilated (mostly ICU) or having very high oxygen requirements on CPAP/NIV masks. Current advice is to wear a full gown, double gloves, surgical scrub hat, N95 mask, face protector and shoe covers.
PP for general COVID contact -> fluid-resistant surgical face mask, plastic apron, gloves.
Pharmacists
Chloe is a Senior Pharmacy Technician, and explained that previously she would split her day between ward based work and education and training. However, now she’s spending the majority of her time on COVID wards. She is working alongside Ward Pharmacists to ensure safe use and supply of medications. They are doing this by working closely with nursing staff to obtain patient information to give the best patient care.
Pharmacists main priorities are;
- For each newly admitted patient, they use various sources to obtain an accurate drug history. Ensuring the safe administration of medications
- They ensure medications are available so that no doses are missed. And that those prescribed are appropriate and safe
- Dispense medications at ward level where possible to ensure patients are discharged as soon as possible without compromising safety
- Dispensing medications for those that are on COVID recovery trials
- Organising patients “TTA’s” (to take away) medications. Currently they’re trying to get patients discharged from hospital quickly to get them home safe. The pharmacists at our hospital are working flat out to organise these.
Paramedics
Faye works as a paramedic and explained that there seem to be changes to PPE regulations regularly. Paramedics are seeing and treating COVID patients at home, Only taking them to the hospital when absolutely necessary. This is for their own safety, and is the same for patients with and without COVID. New pathways for community treatment have opened up recently preventing hospital admissions and improving patient care which is great – ‘some good things happening within this horrific pandemic’.
Operating Department Practitioners
I actually didn’t know about this role before Anita explained what ODP’s do… ‘if there’s an anaesthetic anywhere, we are involved. If there’s any type of surgery, we are involved. And if it’s in the operating room we will know how to use it, fix it, and find it.’
Three weeks ago, Anita and her team were told they would need to work on ITU. They are supported but are expected to take patients, do observations, help with turns, help with personal care. Another team have become the emergency response team. Collecting and transferring patients who become too ill to stay in a ward and need a safe journey to intensive care.
We are not performing elective patient surgery. We have a couple of short notice lists which we treat as infected, so full precautions. Obstetrics is still happening, (you can’t stop the babies!) but they are now confronted with a workforce in PPE not quite the birth experience anyone wants but we make it as nice as we can.
When we give patients anaesthetic, we are always aware that we are the last people they will see and speak to. So we want to make sure everyone feels safe and cared for, no matter the outcome. We are translating that into our patient care now, when they are scared, distressed, and alone.
Dietitians
Dietitians work across almost every ward in the hospital as well as with outpatient via clinics too. (Currently we’ve made all of our clinics telephone based.) On intensive care, many of the patients are intubated and ventilated and so cannot eat at all. We work out their energy (calorie) and protein requirements. And feed them using specially developed nutritional feeds through a Nasogastric tube (NG tube). If they can’t be fed through an NG which goes through the nose into their stomach (the preferred route if a patient has a functioning gut) then they will typically be given parenteral nutrition (PN) which is intravenous nutrition.
When calculating nutrition requirements we take into consideration weight, BMI, age, prior nutritional status, presenting complaint and relevant past medical history, as well as access (eg oral, NG, PN) and the medication they are on. Propofol, a drug used in ICU for sedation, contains calories from fat, and have to be taken into consideration when feeding patients.
Many patients are being ‘prone’ ie lying on their front. Or being tilted to improve breathing, which makes feeding even more difficult in some cases.
“The dietitians goal is to ensure the patient receives the right amount of nutrition to aid recovery from their acute illness and to support their on-going rehab when they recover.” – BDA
For those patients that are not intubated, some are on CPAP masks providing extra oxygen to them. There are some patients, that have very high oxygen requirements that are unable to remove these tight face masks to be able to eat and drink. Our role is to discuss with doctors whether patients are able to meet their nutritional requirements when they take the masks off. We increase nutritional intake during this time with the aid of supplement drinks that are high in calories and protein in small volumes. For those that cannot take their masks off, then we discuss whether NG feeding is the right way to go. Or if we need to look at short term PN.
Dietitians use evidence based guidelines to write and implement feeding protocols. However currently there isn’t a huge amount of research into nutrition for COVID-19 patients. We have had two seminars this week specifically on the topic of nutrition in COVID patients. And we are utilising advice from ESPEN (European Society for Clinical Nutrition and Metabolism) and the BDA Critical Care Best Practice Guidance. As well as discussing treatment options with the respiratory and ICU consultants to make appropriate patient specific plans.
In wards where oxygen use is lower, typically patients are able to eat and drink. However their intake is sometimes lower than usual during admission (and sometimes in the days leading up to hospital admission). We want to maximise nutritional intake for all of our patients. And so we utilise a combination of supplements, fortified snacks and energy dense meals to optimise calorie and protein intake. Working alongside the Speech and Language Team (SALT), we ensure that patients are having the right texture modifications where swallowing is an issue. For example, puree diets or easy to chew foods. These texture modifications can also be useful when patients are lacking energy and finding it difficult to manage normal foods. Opting for smaller, energy dense meals or easy-chew meals reduces the energy required to eat!
Advice and evidence is changing rapidly for Coronavirus. And so we’re trying to keep up to date with the BDA Critical Care guidelines, as well as discussing best practice with other dietitians across the NHS.
Of course, while all of this is going on, we still have non-COVID patients within the hospital and at home that require dietetic input. So we still have dietitians seeing those patients for diabetes advice/education including gestational diabetes , nutrition support, home enteral feeding, coeliac disease education, decompensated liver disease dietary info, renal disease advice, and so much more.
Students
Shout out to the medical students, the nursing student and all those studying healthcare who have volunteered in hospitals when their exams/placements were cancelled.
This is by no means an exhaustive list of the roles of any of the above professions, and I’d love to hear from you if you’re working in one of these jobs or if you’re working front line in a different healthcare role. Thank you to everyone working in essential roles right now!
Other posts you might like:



Incredible! So interesting to read and learn something about what is going on in hospitals today. Sincere thanks to you all. X
Really interesting to see how the wider impact is affecting hospital staff. We hear loads of it in the news, but it often misses the others who work in hospitals.
So incredibly grateful to you and all your colleagues for what you’re doing – more than ever.
Very interesting article. I work as a medical secretary and meet a lot of specialists (physios particularly) but never appreciated what they were all doing in this crisis. Thanks
Thank you! I work as an OT and often feel overlooked. Thank you for recognizing all allied professionals right now
Looking at the work done by the frontline workers & through this post I have become more grateful than ever before
Thank you- a million times over! I am inspired by your courage and commitment to keeping our community safe and healthy.
Thanks for bringing into the picture of the various healthcare professionals who work for avoiding the spread of Covid-19. Hats off to the selfless service of the health care professionals. The job of lab technicians is highly commendable during this situation. Thanks for the informative post.
Yeeeeyyyyy a mention for the ODPs, great blog ???????